Reticulocyte, Absolute
Other names: Retic Ct Abs
Other names: retic count, reticulocyte percent, reticulocyte index, reticulocyte production index, RPI
Reticulocytes are red blood cells that are still developing. They are also known as immature red blood cells. Reticulocytes are made in the bone marrow and sent into the bloodstream. About two days after they form, they develop into mature red blood cells. These red blood cells move oxygen from your lungs to every cell in your body.
A reticulocyte count (retic count) measures the number of reticulocytes in the blood. If the count is too high or too low, it can mean a serious health problem, including:
- anemia
- disorders of the bone marrow, liver, and kidneys.
A reticulocyte count is most often used to:
- Diagnose specific types of anemia. Anemia is a condition in which your blood has a lower than normal amount of red blood cells. There are several different forms and causes of anemia.
- See if treatment for anemia is working
- See if bone marrow is producing the right amount of blood cells
- Check bone marrow function after chemotherapy or a bone marrow transplant
Lab Results Explained and Tracked
What does it mean if your Reticulocyte, Absolute result is too high?
If your results show a higher than normal amount of reticulocytes (reticulocytosis), it may mean:
- You have hemolytic anemia, a type of anemia in which red blood cells are destroyed faster than the bone marrow can replace them.
- Your baby has hemolytic disease of the newborn, a condition that limits the ability of a baby's blood to carry oxygen to organs and tissues.
------------------------------
Acute or chronic bleeding (hemorrhage) or increased RBC destruction (hemolysis) can lead to fewer RBCs in the blood, resulting in anemia. The body compensates for this loss or to treatment of deficiency anemias (such as iron deficiency anemia or pernicious anemia) by increasing the rate of RBC production and by releasing RBCs sooner into the blood, before they become more mature. When this happens, the number and percentage of reticulocytes in the blood increases until a sufficient number of RBCs replaces those that were lost or until the production capacity of the bone marrow is reached.
------------------------------
In general, the reticulocyte count (absolute number or percentage) is a reflection of recent bone marrow activity. Results may indicate whether a disease or condition is present that is generating an increased demand for new RBCs and whether the bone marrow is able to respond to the extra requirement. Occasionally, results may indicate overproduction of RBCs.
When anemia is present (i.e., low RBCs, low hemoglobin, low hematocrit) and the bone marrow is responding appropriately to the demand for increased numbers of RBCs, then the bone marrow will produce more and allow for the early release of more immature RBCs, increasing the number of reticulocytes in the blood.
A high reticulocyte count with low RBCs, low hemoglobin, and low hematocrit (anemia) may indicate conditions such as:
- Bleeding: If you bleed, then the number of reticulocytes will rise a few days later in an attempt to compensate for the red cell loss. If you have chronic blood loss, then the number of reticulocytes will stay at an increased level as the marrow tries to keep up with the demand for new RBCs (although it may not be high if the blood loss leads to iron deficiency).
- Hemolytic anemia: In this condition, anemia is caused by increased destruction of RBCs. The bone marrow increases RBC production to compensate, resulting in a high reticulocyte count.
- Hemolytic disease of the newborn: This condition causes increased RBC destruction, similar to hemolytic anemia described above.
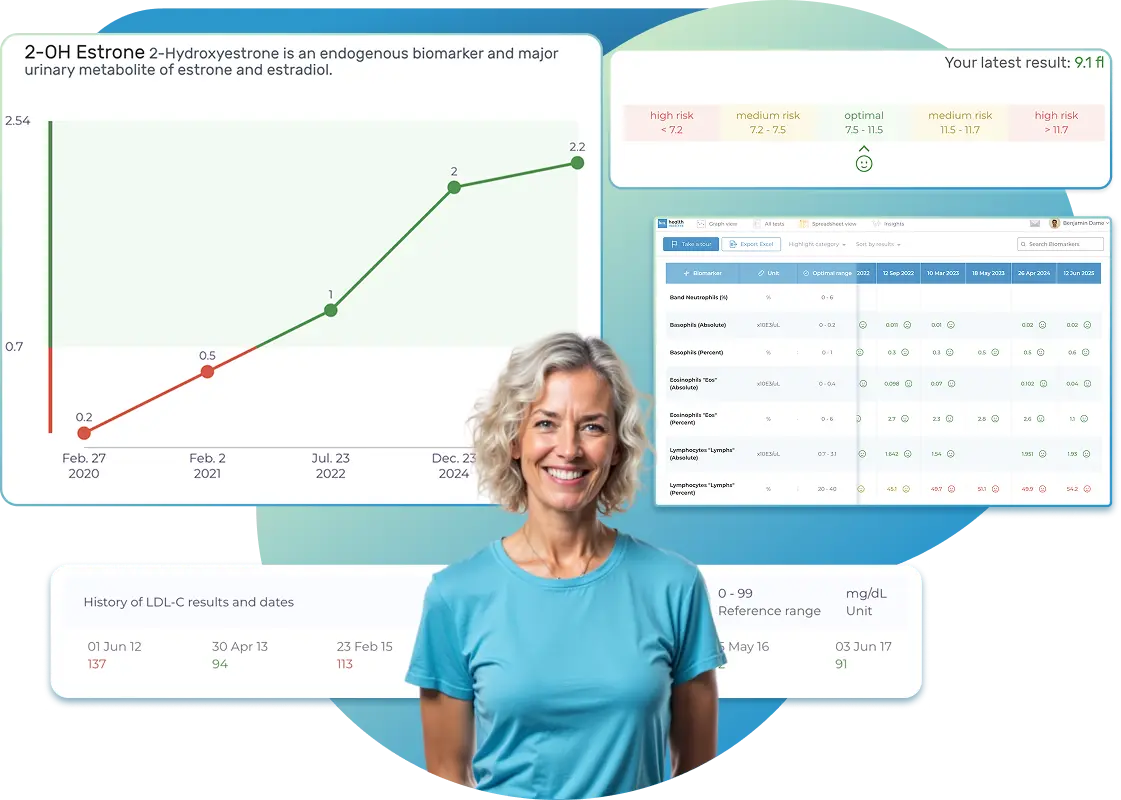
All Your Lab Results.
One Simple Dashboard.
Import, Track, and Share Your Lab Results Easily
Import, Track, and Share Your Lab Results
Import lab results from multiple providers, track changes over time, customize your reference ranges, and get clear explanations for each result. Everything is stored securely, exportable in one organized file, and shareable with your doctor—or anyone you choose.
Cancel or upgrade anytime
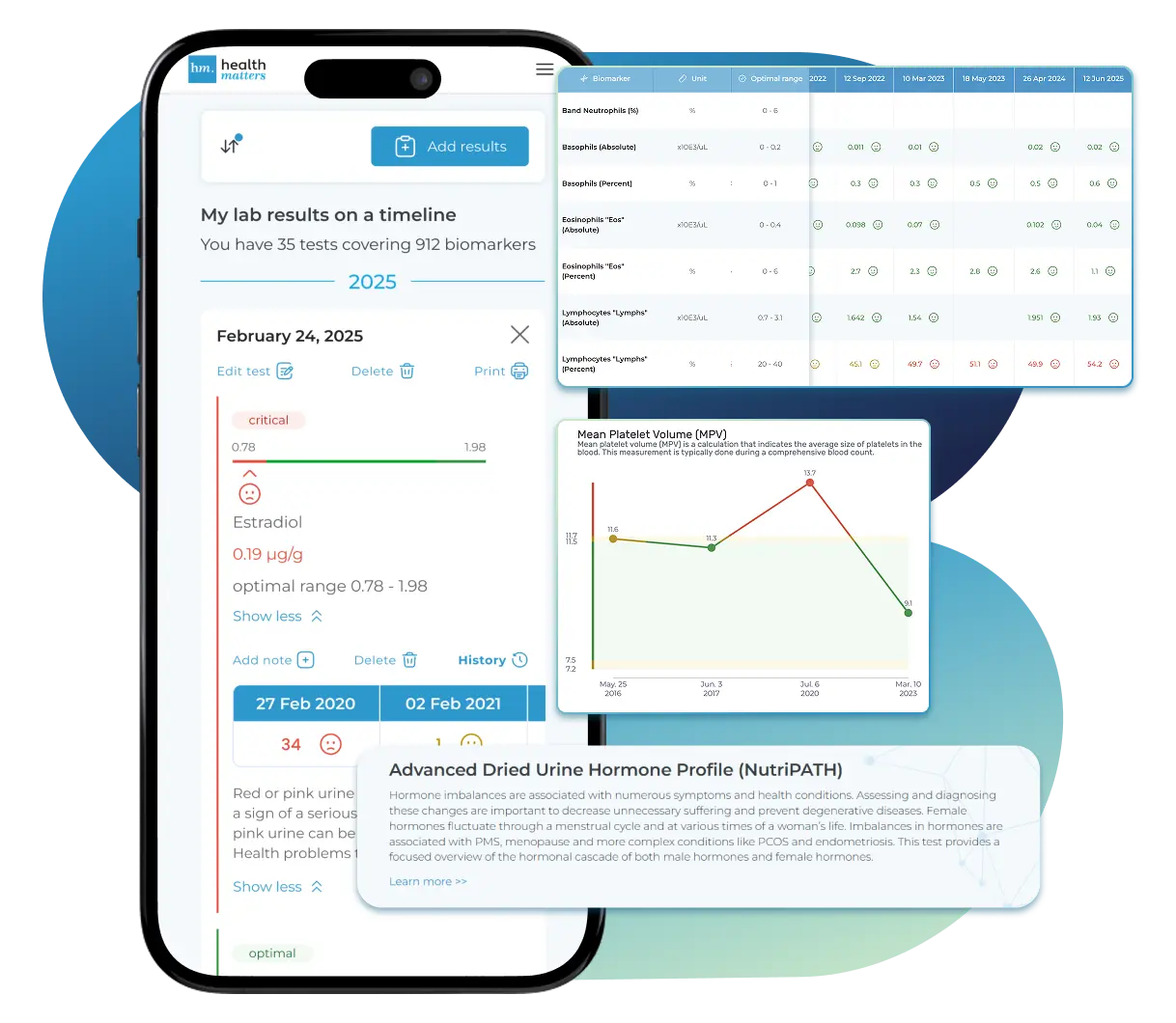
What does it mean if your Reticulocyte, Absolute result is too low?
If your results show a lower than normal amount of reticulocytes, it may mean you have:
- Iron deficiency anemia, a type of anemia that happens when you don't have enough iron in your body.
- Pernicious anemia, a type of anemia caused by not getting enough of certain B vitamins (B12 and folate) in your diet, or when your body can't absorb enough B vitamins.
- Aplastic anemia, a type of anemia that happens when the bone marrow isn't able to make enough blood cells.
- Bone marrow failure, which may be caused by an infection or cancer.
- Kidney disease
- Cirrhosis, scarring of the liver
------------------------------
Decreased RBC production may occur when the bone marrow is not functioning normally. This can result from a bone marrow disorder such as aplastic anemia. Diminished production can also be due to other factors, for example, cirrhosis, kidney disease, radiation or chemotherapy treatments for cancer, a low level of the hormone erythropoietin, or deficiencies in certain nutrients such as iron, vitamin B12 or folate. Decreased production leads to fewer RBCs in circulation, decreased hemoglobin and oxygen-carrying capacity, a lower hematocrit, and a reduced number of reticulocytes as old RBCs are removed from the blood but not fully replaced.
Occasionally, both the reticulocyte count and the RBC count will be increased because of excess RBC production by the bone marrow. This may be due to an increased production of erythropoietin, disorders that cause chronic overproduction of RBCs (polycythemia vera), and cigarette smoking.
Some drugs may increase or decrease reticulocyte counts.
------------------------------
A low reticulocyte count with low RBCs, low hemoglobin, and low hematocrit (anemia) may be seen, for example, with:
- Iron deficiency anemia
- Pernicious anemia or folic acid deficiency
- Aplastic anemia
- Radiation therapy
- Bone marrow failure caused by infection or cancer
- Severe kidney disease; this may cause a low level of erythropoietin.
- Alcoholism
Article Review & Sources
All our content is backed by peer-reviewed studies, academic research, and trusted medical sources. We're committed to accuracy and transparency — see our editorial policy for details.
Laboratories
Bring All Your Lab Results Together — In One Place
We accept reports from any lab, so you can easily collect and organize all your health information in one secure spot.
Pricing Table
Gather Your Lab History — and Finally Make Sense of It
Finally, Your Lab Results Organized and Clear
Personal plans
$79/ year
Advanced Plan
Access your lab reports, explanations, and tracking tools.
- Import lab results from any provider
- Track all results with visual tools
- Customize your reference ranges
- Export your full lab history anytime
- Share results securely with anyone
- Receive 5 reports entered for you
- Cancel or upgrade anytime
$250/ once
Unlimited Account
Pay once, access everything—no monthly fees, no limits.
- Import lab results from any provider
- Track all results with visual tools
- Customize your reference ranges
- Export your full lab history anytime
- Share results securely with anyone
- Receive 10 reports entered for you
- No subscriptions. No extra fees.
$45/ month
Pro Monthly
Designed for professionals managing their clients' lab reports
- Import lab results from any provider
- Track lab results for multiple clients
- Customize reference ranges per client
- Export lab histories and reports
- Begin with first report entered by us
- Cancel or upgrade anytime
About membership
What's included in a Healthmatters membership
 Import Lab Results from Any Source
Import Lab Results from Any Source
 See Your Health Timeline
See Your Health Timeline
 Understand What Your Results Mean
Understand What Your Results Mean
 Visualize Your Results
Visualize Your Results
 Data Entry Service for Your Reports
Data Entry Service for Your Reports
 Securely Share With Anyone You Trust
Securely Share With Anyone You Trust
Let Your Lab Results Tell the Full Story
Once your results are in one place, see the bigger picture — track trends over time, compare data side by side, export your full history, and share securely with anyone you trust.





Bring all your results together to compare, track progress, export your history, and share securely.
What Healthmatters Members Are Saying
We implement proven measures to keep your data safe.
At HealthMatters, we're committed to maintaining the security and confidentiality of your personal information. We've put industry-leading security standards in place to help protect against the loss, misuse, or alteration of the information under our control. We use procedural, physical, and electronic security methods designed to prevent unauthorized people from getting access to this information. Our internal code of conduct adds additional privacy protection. All data is backed up multiple times a day and encrypted using SSL certificates. See our Privacy Policy for more details.

















